Emilio González Martínez (1); Eugenio Cárdenas Ruiz-Valdepeñas (2); Jose García Cosamalón (1); Javier Abarca Olivas (3); Milton M. Rastelli Jr., MD (4)
(1) Department of Neurosurgery, Hospital Universitario de León. León, Spain.
(2) Department of Neurosurgery, Hospital Virgen del Rocío. Sevilla, Spain.
(3) Department of Neurosurgery, Hospital General Universitario de Alicante. Alicante, Spain.
(4) Department of Neurosurgery, Hospital Universitário Cajuru – Pontifícia Universidade Católica do Paraná. Curitiba, Brasil.
Introduction
The Far-lateral approach has been used to approach for the majority of the lesions located ventrolateral to the brainstem and in the upper cervical spinal cord.
This approach pursues to remove the occipital bone including the posterior aspect of the ipsilateral condyle and posterior arch of C1. Anatomical landmarks may be recognized for the neurosurgeon to avoid neurovascular injuries, specially to the vertebral artery and hypoglossal nerve.

The occipital condyles are the contact area of the occipital bone with the articular aspects of C1. They present a inferior convex surface, and they are usually associated to a posterior foramen to the posterior condyle vein.

The hypoglossal cannal penetrates the occipital condyle in its base. It presents a posterior to anterior and a medial to lateral orientation, where hypoglossal nerves cross and leave the intracranial compartment. The intracranial exit zone is 8mm ventral to the posterior aspect of the occipital condyle, and 21mm dorsal to the anterior aspect. The hypoglossal nerve is directed anteriorly and laterally at a 45-degree angle with the sagital plane. The lateral aspect of the intracranial limit is reached removing of approximately the posterior third of the occipital condyle.

Medial view of the Hypoglossal canal: Foramen Magnum.
Step 0: Position
The patient is positionated in a park bench. The head is flexed until the chin is one centimeter from the sternum, rotated contra-laterally to the lesion, and flexed 30-degree laterally toward the contralateral shoulder, allowing to increase the angle between the atlas and foramen magnum.
Step 1: Skin
Step 1A

We must indentify three important landmarks: the external occipital protuberance, the mastoid process…
Step 1b

…And the transverse process of C1 which may be touched in the middle way between the mastoid tip and the posterior angle of the mandible.
Step 1c

The scalp should be performed with an inverted horseshoe incision. It begins 5cm below the external occipital protuberance and ascends above the superior nuchal line on the midline. Subsequently, it descends in front of the posterior border of the sternocleidomastoid muscle and ends 5cm below of the lateral mass of C1.
In the neurosurgical practice, the scalp and muscles are reflected together. However, they have been reflected separatetly for teaching purposes.
Step 2: Muscle
Step 2a


The muscle dissection is usually performed in one layer, but in this case layer-by-layer has been done for teaching purposes. Initially, after the skin and subcutaneous is everted, a superficial fascia is exposed, where the superficial occipital artery is located.
Step 2b

The sternocleidomastoid, laterally, and trapezious muscle, medially, constitute the first muscular layer. The sternocleidomastoid muscle presents superiorly an attachment in the mastoid tip and in the lateral part of the superior nuchal line, and it is directed downward and anteriorly to the clavicle and the manubrium sterni. The trapezius muscle is attached in the superior nuchal line, the external occipital protuberance and the posterior cervical ligament.
Step 2c

The splenius capitis muscle is located under the sternocleidomastoid muscle. It is attached in the mastoid tip and is directed downward and medially to the inferior half of the ligamentum nuchae. The semispinalis capitis muscle is located medially and under the splenius capitis muscle. It is attached between the superior and inferior nuchal lines and courses inferiorly to the transverse process of C4, C5 and C6.
Step 2d

The occipital artery is visibe after detaching the splenius capitis muscle. It is a branch from the external carotid artery, and it usually emerges 20 mm further the carotid bifucartion at the level of the angle of the mandible. It ascends and goes backward, first between the rectus capitis lateralis and later between the superior oblique and the posterior aspect of the digastric muscle. It is accompanied by the occipital vein. It presents two possible ways according to the presence of the occipital groove, located medial to the mastoid notch. If it is absent, the artery courses superficial to the longissimus capitis muscle or coursing deeply to it if the groove is patent.
Step 3: The suboccipital triangle
Step 3a
 The suboccipital triangle is covered by a layer of dense fibrofatty tissue. It is formed superolaterally by the superior oblique muscle and inferiorly by the inferior oblique muscle, and medially by the rectus capitis posterior major. It contains the horizontal portion of the vertebral artery and the C1 nerve, lying in a groove on the upper surface of the lateral part of the posterior arch of the atlas.
The suboccipital triangle is covered by a layer of dense fibrofatty tissue. It is formed superolaterally by the superior oblique muscle and inferiorly by the inferior oblique muscle, and medially by the rectus capitis posterior major. It contains the horizontal portion of the vertebral artery and the C1 nerve, lying in a groove on the upper surface of the lateral part of the posterior arch of the atlas.
Step 3b

This is a view after opening of the suboccipital triangle and removing the lateral aspect of C1 and C2 laminas.
Step 3c

The segment of the vertebral artery located between the C1 transverse process and the dural entrance gives rise to muscular branches and the posterior meningeal artery, which can be safely coagulated. The PICA ocasionally arises extradural and could be inadvertently injured.
Step 3d: Vertebral artery transposition

The vertebral artery transposition makes the condylar drilling easier and safer. For the vertebral artery transposition is necessary to open the foramen transverse of C1 and mobilize the artery inferomedially .
Step 4: Craniotomy

The suboccipital craniectomy is performed from the inferior nuchal line, superiorly, to the posterior rim of the foramen magnum, inferiorly, and up to the occipital condyle laterally .
Step 5: Intradural anatomy
Step 5a: opening the dura

A curvilinear incision of the dura is performed just from behind of the sigmoid sinus to the C2 lamina, and it is reflected and held medially and laterally with sutures. The opening may be extended up to the junction of sigmoid and transverse sinus if cerebello-pontine angle has to be approached.
Step 5b: before drilling the condyle

Although the dural opening is performed after drilling of the occipital condyle, it has been opened before to expose the neurovascular structures. The hypoglossal nerve arises from the preolivar sulcus and runs laterally to the hypoglossal canal. From this view, the hypoglossal nerve is covered by the roots of the accesory nerve.
Step 5c: after drilling the condyle
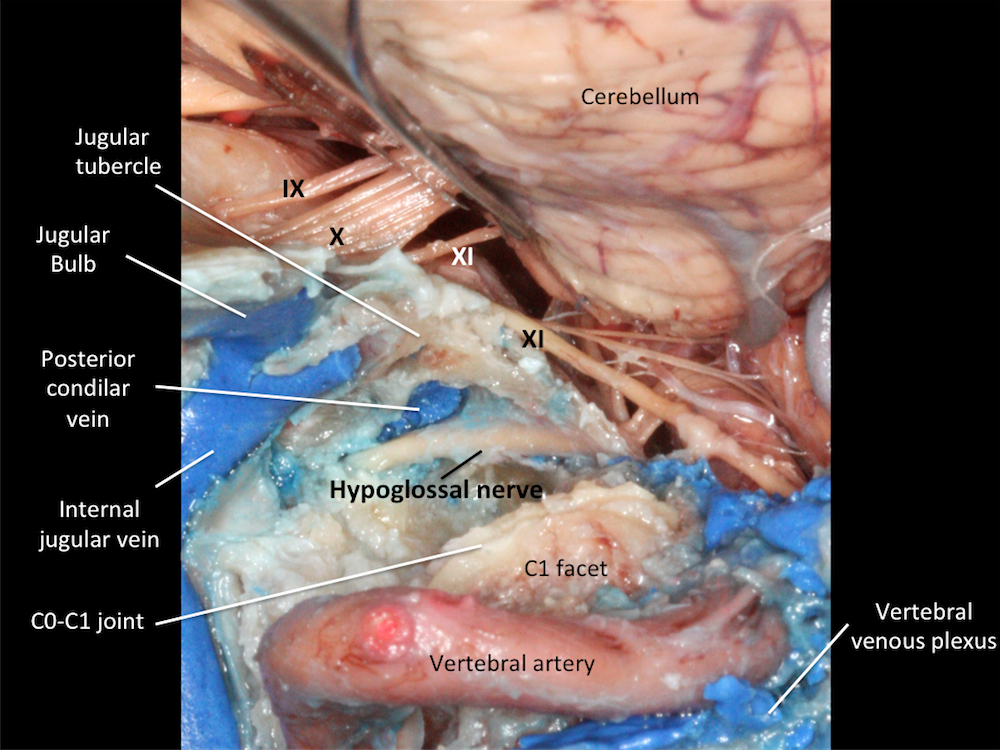
The posterior condylar emissary vein, which travels from the jugular bulb to the extradural venous plexus, may be injured and hemostasis, if it is necessary. The degree of occipital condyle removal vary widely, although posterior and medial one third of the condyle usually is enough for ventrolateral tumors. If more than 50% of the condyle is resected, the craniovertevral junction becomes unstable, and occipitocervical stabilization is required.
Step 5d: the CPA from the far lateral approach
References
Lanzino G, Paolini S, Spetzler RF: Far-lateral approach to the craniocervical junction. Neurosurgery 2005, 57:367-371; discussion 367-371.
Rhoton AL, Jr.: The far-lateral approach and its transcondylar, supracondylar, and paracondylar extensions. Neurosurgery 2000, 47:S195-209.
Liu JKL, Rao G, Schmidt MH, Couldwell W: Far lateral transcondylar transtubercular approach to lesions of the ventral foramen magnum and craniovertebral junction. Contemporary Neurosurgery 2007, 29 (10)
Acknowledgements
Thanks to Juan Carlos Fernández Miranda, director of the Surgical Neuroanatomy Laboratory at the University of Pittsburgh School of Medicine (Pittsburgh, Pennsylvania, US), for providing the cadaveric specimenes.








Follow us